You may have heard about a link between grain-free diets and canine heart disease from the news or from your veterinarian. If you haven’t, here’s some important information we’d like to share with you:
The U.S. Food and Drug Administration has alerted pet owners and veterinary professionals about reports of canine dilated cardiomyopathy (DCM) in dogs that are eating grain free foods. It should be noted that cats eating similar foods are at an even greater risk.
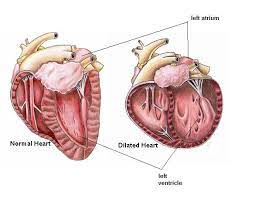
Canine dilated cardiomyopathy (DCM) is a heart muscle disorder that results in a decreased ability of the heart to pump blood through the body. Historically, this seemed to be a heritable disease affecting certain dog breeds.
Previously, cats eating certain diets came down with this disorder. Once dietary changes were made by food companies, we stopped seeing this in cats and only specific dog breeds, most notably the Doberman Pincher, Boxers, Irish Wolfhounds and Great Danes.
More recently, with the advent of grain-free / boutique diets, veterinary cardiologists began reporting the disease in atypical dog breeds.
The FDA stated in its report in July that the Center for Veterinary Medicine is looking into the links between grain-free dog foods and DCM along with the Veterinary Laboratory Investigation and Response Network.

Recently, veterinary cardiologists have been reporting increased rates of DCM in breeds not usually associated with DCM such as Miniature Schnauzers, Golden Retrievers, Labrador Retrievers, Doodle mixes, Shih Tzus and French Bulldogs.
There is suspicion that the disease is associated with eating boutique or grain-free diets with some of the dogs improving when their diets are changed.
A cardiologist from North Carolina State College of Veterinary Medicine noted DCM in a household with two unrelated Miniature Schnauzers and they were both eating the same boutique, exotic protein grain free diet.
Cardiologists have noticed that both the typical and atypical breeds were more likely to be eating boutique or grain-free diets with ingredients such as kangaroo, lentils, duck, pea, fava bean, buffalo, tapioca, salmon, lamb, barley, bison, venison, and chickpeas.

Some vegan diets have been associated with DCM and it has even been seen in dogs eating raw or home-prepared diets.
The cause of the rise in DCM in breeds not usually associated with this condition is unclear at this time. The most likely opinion is related to the amino acid taurine.
While most grain-free foods have it, there may be a problem with how its processed and absorbed in the grain-free diets. Taurine is an essential amino acid involved in heart contractility.
We learned this lesson the hard way when DCM was found in cats. In 1987 it was discovered that feline DCM was caused by insufficient taurine in the diet.
All reputable commercial cat foods now contain enough taurine to prevent the development of this lethal disease.

While no one is 100% certain why the grain-free diets are causing DCM, it is suspected that there is a link to how the taurine is processed. Most of the atypical dogs affected were eating boutique, grain free or exotic ingredient diets. Many affected dogs improved with taurine supplementation and returning them to a traditional grain diet.
If you are feeding your dog or cat a grain-free or raw diet, it is recommended that you switch back to a traditional grain fortified diet. In fact, there is no proven benefit to feeding a diet that lacks grains.

So what is the best diet for your pets? You can speak with your veterinarian about what diet is most appropriate. based on your pet’s age, level of activity, and any special needs or requirements they may have.
The right nutrients in the right proportions must be in the diet, the effects of processing (or not processing) the food needs to be considered, and the effects all the other ingredients in the food need to be addressed, in addition to ensuring rigorous quality control and testing.
Not every manufacturer can do this type of quality control and food analysis/testing and certainly not every manufacturer does.
If your pet is in good health and a good body weight, some very reputable brands that put a lot of research into their foods include Royal Canin, Hills, Eukanuba and Purina. These diets are readily available in pet food stores and some are even found in supermarkets.


