It is a common human ailment and has in the past been considered to be the most common hormone imbalance of dogs, though this has lately been called into question as test results can be confusing. It seems like hypothyroidism would be a straight forward condition: the body does not produce enough thyroid hormone, disease results, a test shows thyroid hormone level is low, additional hormone is taken as a pill, problem solved. This article attempts to review the issues relevant to this condition and the pitfalls that keep it from being a simple problem.
Thyroid hormone is often described as the volume dial of the body’s metabolism. Every cell in the body is affected by it. Too much hormone and the heart races, blood pressure rises, and muscle and fat are burned until the patient becomes skinny and debilitated. Too little hormone and the patient becomes listless, overweight, and even bald in spots. Hypothyroidism is the medical condition where the body is deficient in thyroid hormone. It would seem simple enough to identify patients with hypothyroidism, test them, treat them and watch them return to normal. Unfortunately, it is not as easy to identify affected patients as it might sound. Let’s review the issues relevant to this condition and the pitfalls that keep it from being a simple problem.
What is the Thyroid Gland and What Does it do?
Production of T4 is regulated by the pituitary gland at the base of one’s brain. (This gland is called the master gland as it regulates hormone production in the adrenal system, the thyroid system, the reproductive system and more). The pituitary produces a substance called thyroid stimulating hormone (TSH). When T4 levels are dropping, the pituitary gland stimulates the thyroid gland to make and release more T4.The thyroid gland forms an H in one’s throat as show in the graphic above, though in dogs, the thyroid exists as two separate halves. The thyroid produces two forms of thyroid hormone: T3, which is the active form of the hormone; and T4, which is the inactive form created to circulate in the bloodstream. When T4 is absorbed into tissue cells, it is converted into T3. Most of the circulating T4 is carried by blood proteins and is not available for tissue absorption; the portion that is not carried by proteins (the so-called free T4) is the portion that is able to enter tissues for activation. The thyroid gland itself can also activate T4 into T3. In dogs about half of the T3 comes from the thyroid gland and the other half comes from the body’s other tissues. In humans, 80 percent of T3 comes from activation in the body’s other tissues.
Active thyroid hormone serves as a sort of a volume dial for metabolism. Since virtually every cell in the body can be affected by reduced levels of thyroid hormone, it is not surprising that reduced levels of thyroid hormone lead to symptoms in multiple body systems.
Manifestations of Hypothyroidism
In short, hypothyroidism is the natural deficiency of thyroid hormone. This deficiency is produced by immune-mediated destruction of the thyroid gland, by natural atrophy of the gland, by dietary iodine deficiency, or as a congenital problem. In dogs, the first two causes listed account for almost all cases, though currently the feeling is that atrophy of the gland actually represents the end result of earlier immune-mediated destruction of the gland.
Hypothyroidism generally develops in middle aged or elderly dogs. Breeds with definite predisposition to develop hypothyroidism include: the Doberman pinscher, the Golden retriever, the Irish Setter, the Great Dane, the Dachshund, and the Boxer.
Hypothyroidism is a classical disease with a classical collection of clinical signs. One particularly well-done survey of 162 confirmed hypothyroid dogs showed the following common findings:
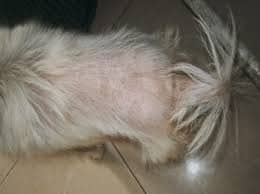
- 88% had some kind of skin abnormality
- 40% had hair loss (often this starts on the tail leading to a rat tail appearance or a bald area around the collar.)
- 22% had skin infection (often dogs are scaly and smelly due to an excessively oily coat.)
- 14% had brittle or dry coats (often the outer hairs break off leaving a short, softer under coat, classically described as a puppy-like coat.)
- 49% were obese
- 48% were described as lethargic or listless at home
- 36% were anemic (had a reduced number of red blood cells due to slowed red blood cell production in the bone marrow.) Elevated blood cholesterol levels are also considered a common finding of hypothyroidism.
One classical finding in hypothyroid dogs is a thickening of some tissues, especially of the face and head. The skin in particular thickens, leading to more skin folds and what is referred to as a tragic face. This thickening can occur in some other tissues as well (such as facial nerves – see below).
Cardiovascular Signs
Hypothyroidism interferes with the electrical fibers that more or less provide the wiring for the heart. The rhythmic contractions of heart muscle are normally stimulated by these electrochemical fibers. Abnormal rhythms or slow heart rate occur in as many as 26% of hypothyroid dogs; still, the significance of this in terms of overall lifestyle is not clear. Many specialists feel thyroid supplementation should be started at a lower dose for patients with obvious heart disease.
Neurologic Signs
According to surveys of confirmed hypothyroid dogs, only about 2 to 4 percent have nerve problems. There are several syndromes reported.
- Polyneuropathy – In hypothyroidism, nerves simply do not conduct electrical impulses normally. This may account for some of the general weakness and listlessness seen in hypothyroidism. Response to thyroid hormone therapy is rapid (improvement within the first week of treatment).
- Focal Neuropathy – Single nerves can get entrapped as they exit the skull or spinal cord as they (like other tissues) swell with thickening. Pressure on these nerves can lead to paralysis of the facial muscles and/or head tilt, bizarre eye motions and balance disruption (vestibular disease)
- Central Nervous System – may represent abnormal electrical conduction within nerves; however, vascular disease has been found in hypothyroid dogs with central nervous system signs. Clinical signs have involved ataxia (drunken gait), hemiparesis (weakness in front and back legs on the same side of the body), hypermetria (inappropriate measurement of steps), head tilt, circling and cranial nerve abnormalities. It may take several months of therapy to see a response. Coma from thickening in the brain’s tissues is a rare possibility but has been known to occur.
Ocular (Eye) Signs
Ocular changes are not common in hypothyroidism but the high levels of blood cholesterol and circulating fat can sometimes lead to eye changes. When these changes are seen, often thyroid testing is recommended. Corneal dystrophy, an abnormal change in the clear covering of the eye, is such an eye sign. This finding is usually represented as a small white spot (sometimes a white circle) on the eye surface. At this degree it is only a cosmetic problem and does not interfere with vision. In more severe forms, painful bubbles can erupt on the corneal surface that lead to ulceration. Obviously, this form would require treatment.
Conditions not proven but previously suspected to be associated with hypothyroidism include: megaesophagus, laryngeal paralysis, infertility, and behavioral aggression.
Testing for Hypothyroidism
You would think testing for hypothyroidism would be simple: a blood test of the T3 or T4 level could be checked and if it is low, the patient is hypothyroid. Unfortunately, the situation is rarely so simple.
Measurement of T3
If T3 is the active hormone, why can’t we just test blood levels of T3? Due to assorted compensatory mechanisms, T3 levels often fluctuate into the normal range in even truly hypothyroid dogs. This means that T3 values are virtually useless in diagnosing hypothyroidism.
Measurement of T4
The T4 level (also called the total T4 level) is included in many routine screening blood panels. It would seem that a low T4 would indicate hypothyroidism and a normal T4 would indicate normal thyroid function. Unfortunately, it isn’t that simple. Dogs on certain drugs (most notably seizure medications phenobarbital and potassium bromide; prednisone or other corticosteroids; non-steroidal anti-inflammatory drugs or NSAIDs; a heart medication called propranolol; a behavior medication called clomipramine; or sulfa class antibiotics) or with illnesses other than thyroid disease often have depressed T4 secretion. These dogs will have low T4’s but are not hypothyroid. This means a normal T4 indicates normal thyroid function but a low T4 may or may not indicate hypothyroidism. There is also a grey zone where T4 results are considered not definitively normal and not definitively abnormal. In short, T4 alone is not adequate to make a diagnosis of hypothyroidism.
It should be noted that the sighthounds normally have much lower T4 levels than other breeds. In Greyhounds, for example, the T4 levels typically run about 50% of what other breeds do. Interestingly, their T3 levels have the same normal range as other breeds.
Free T4 levels are typically 1000 times smaller than total T4 levels plus tests for free T4 have to work in such a way so as not to convert bound T4 into free T4 and thus interfere with results. Because of these two issues, it is somewhat difficult to test for free T4 and the only acceptable way to do this is by a method called equilibrium dialysis. At this time most labs offer equilibrium dialysis free T4 but it is important to realize that a free T4 level on a lab report is not an equilibrium dialysis free T4 unless it specifically says so. Equilibrium dialysis free T4 is sometimes notated fT4(ED).Free T4
As mentioned, T4 is the precursor hormone that is not active but is converted by body tissues into T3, which is active. T4 exists in two forms: the form carried around bonded to a blood protein (this is called bound T4) and T4 floating around loose in the bloodstream (called free T4). Only free T4 can enter cells and be converted to T3 and the concentration of free T4 corresponds to thyroid hormone activity where it counts (i.e., at the tissue level). Free T4 levels are less subject to fluctuate into a falsely low range in response to non-thyroidal diseases or drugs than is a total T4 level.
TSH Stimulation and Endogenous TSH levels
Before there was readily available equilibrium dialysis free T4, the test that was felt to be the gold standard of reliability was called the TSH stimulation test. In this test, a T4 was measured and then compared with a value drawn 8 hours after an injection of thyroid stimulating hormone (TSH). Inability to respond to TSH was considered indicative of hypothyroidism. The problem was expense, the need for 8 hours of hospitalization, and the fact that injectable TSH was frequently off the market. This test is rarely performed nowadays.
TSH can be directly measured in a patient’s bloodstream. The idea is that the pituitary gland should be secreting high levels of TSH in a futile attempt to stimulate a diseased thyroid gland. Measurement of TSH level is an important means of diagnosing hypothyroidism in humans and a canine version of the test was long sought. Unfortunately, when it finally became available, it was found that many dogs (approximately 25%) with true hypothyroidism did not have elevated TSH levels as one would expect; still, this test is often helpful in making the diagnosis of hypothyroidism.
Antithyroglobulin Antibodies (The TGAA test)
Some thyroid testing panels include a measurement of antibodies against the thyroid gland proteins from which thyroid hormones are made. The presence of these antibodies confirms the immune-mediated form of hypothyroidism (though in later stages of this disease antibodies are no longer produced). The only significance of this test other than academic interest is to identify patients that are positive for antibodies yet have normal thyroid hormone tests. These animals have a 20% chance of becoming hypothyroid later on, so regular periodic testing of thyroid hormone levels would be a good idea. Treatment of hypothyroid animals that are positive for antibodies is the same as treatment for that that are antibody negative; the only practical use of the test is to identify animals at risk for becoming hypothyroid later on.
Testing with a Trial of Medication
Sometimes the only way to test for hypothyroidism is to simply give the medication for several months and see what happens. Often an improvement in attitude and energy level is seen within the first week. Hair re-growth takes substantially longer (typically 4 months minimum) as the follicles must reawaken and then grow a hair long enough to be seen.
Is the Diagnosis Correct?
Because of difficulties in diagnostic testing methods many dogs have been erroneously diagnosed with hypothyroidism and have been on medication for years. If there is any question about a patient and you wish to re-test, thyroid hormone supplementation must be discontinued at least 2 months for blood testing to be valid. If possible, medications known to interfere with testing should be discontinued for testing (though this is obviously not always possible).
Treatment of Hypothyroidism
At least treatment of hypothyroidism is relatively straight forward; hypothyroidism is treated with oral administration of thyroid hormone (T4). Even hypothyroid dogs are perfectly capable of converting T4 to T3. Pills are given usually twice daily to start but may be dropped to once a day after good thyroid control has been achieved.
There are many brands of thyroid supplementation available and prices are somewhat variable depending on the manufacturer.
Treatment is given for the rest of the dog’s life.
Occasionally veterinarians are asked if it is reasonable to use dried or powdered thyroid glands of hogs or cattle as a more natural form of treatment. The answer is simply no. These products are not produced with adequate quality control to ensure that they contain a reliable amount of thyroid hormone. Each dose may be completely different when such a product is used.
Re-testing later on
Whenever an animal goes on a medication long term, periodic blood testing is a good idea. In the case of hypothyroidism treatment, it is important to know if the medication dose is too low or too high. Thyroxine (T4) is a safe medication but if it is not given in adequate doses, obviously the patient will not be adequately treated. If the dose is too high and given for too long a time, excessive water consumption, weight loss, and restlessness can result.