
Your pet’s immune system is an intricate machine that allows it to determine what to allow in the body and what to fight off. Usually, it does its job well, but when it malfunctions, thing can get messy fast and an auto-immune disease occurs.
When an auto-immune process happens, it means the immune system doesn’t work the way it is supposed to and can attack cells in an animal’s own body. Basically, the immune system decides that something harmless is dangerous and it goes into action and attacks it as if it were a dangerous invader.
Examples of autoimmune diseases include rheumatoid arthritis, lupus, and diabetes mellitus in dogs.
One of the more common autoimmune diseases that veterinarians see is immune-mediated hemolytic anemia, or IMHA. Here, the immune system decides that red blood cells are harmful and starts destroying them. In many cases the incting trigger is never known. The ‘hemolytic’ in the name refers to the process of popping, or lysing, red blood cells. Incidentally, onions, mothballs, and the zinc found in pennies minted after 1982 can all cause the same thing.
Some of the signs of IMHA include:
- Pale or yellow gums
- Extreme weakness and lethargy
- Loss of appetite
- Jaundice (yellow discoloration) of the whites of the eyes.
It can happen with remarkable speed – one day your dog is happily snoozing by the fire, the next day your veterinarian is telling you that he’s in a 50:50 battle for his life. The speed with which this occurs is horrifyingly fast. An immune system reacts efficiently even to dangers that are not real.
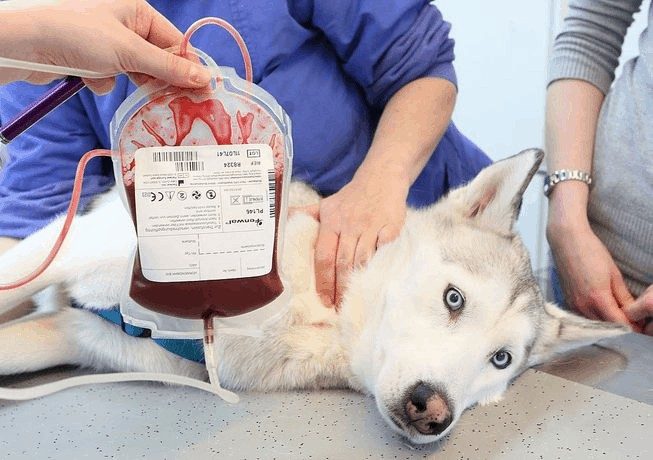
IMHA and its close cousin Evan’s syndrome (in which red blood cells and platelets are both consumed) are not easily treated. The odds of survival are around 50:50. Doing battle with the immune system is not for the faint of heart or with financial restraints. Treatment includes many days in the hospital, multiple blood transfusions and expensive medications – adding quickly to the tune of thousands. Some owners due to cost are unable or elect not to go ahead with therapy.
One of the worst consequences of IMHA is a blood clot that can travel to the lungs and is often fatal: a pulmonary thromboembolism. This is a consequence of hyperactive clotting associated in the disease and can occur in animals that seem to be recoveing.
Pets who survive are on medication for months (steroids such as prednisone are the cornerstone of therapy) and about one dog in five will relapse at some point. Cats are comparatively resistant to IMHA; they can still get it, but it’s common to see hundreds of dog cases and only a handful of cats.
There is an association between recent vaccination and the onset of IMHA, but that does not infer that vaccines cause IMHA. It’s just not that simple. Almost anything that ramps of the immune system in an animal prone to have an immune-mediated disease can cause this devesation. Vaccinations are only one of many underlying causes. Far more animals die from diseases like parvovirus and panleukopenia because they are not vaccinated vs the very rare few that develop an auto-immune complication.
We do, however, usually recommend that patients who have had IMHA not receive vaccinations ever again in the future, out of an abundance of caution.
Other things that trigger the immune dysfunction in predisposed individuals are certain drugs, tick-borne diseases and cancer.
