Arthritis or degenerative joint disease (DJD), is a degenerative, progressive, and irreversible condition of the joints. It is characterized by the progressive loss of joint cartilage, bony spurs/growths, and the thickening and scarring of connective tissue around the joint, usually as a result of injury.

Approximately 25 percent of dogs are diagnosed with arthritis in their life time, and as many as 60 percent of dogs have radiographic evidence of it.
Degenerative joint disorders are probably as common in cats as in dogs but are less likely to be associated with obvious clinical signs, such as lameness. In one study, 90 percent of cats over 12 years of age had radiographic signs of osteoarthritis.
Arthritis is classified as primary or secondary. Primary arthritis is associated with aging, due to years of wear and tear on the joints. Secondary arthritis is the result of an external event or force (e.g., trauma, poor joint alignment, etc.) that once damaged the joint cartilage.
Arthritis can affect any age, sex, and breed of dog and cat. Most predispositions to it relate to underlying causes, such as elbow dysplasia, hip dysplasia, osteochondrosis, and so forth.
Diagnosis

Diagnosis is based on what is found in the physical examination, diagnostic imaging, joint taps, cytology, force plate gain analysis, therapeutic drug trials, and other tests.
Physical Examination Findings in Dogs
Lameness is the most common sign. It may happen once in a while (episodic) progressive (gets worse over time), or be persistent. Stiffness is common after periods of rest. Stiffness and lameness may decrease when the dog warms up a bit with some activity. Lameness often gets worse after periods of overexertion.
Pain, swelling, and decreased range of motion may be seen. Thickened joints, excess fluid in the joint space, and muscle weakening are likely to occur.

Physical Examination Findings in Cats
As opposed to the visible lameness seen commonly in dogs, many cats simply become less active, may hide, or develop behavioral changes, such as irritability, decreased grooming, or difficulty getting into position in the litterbox.
Cats also may have joint swelling/thickening, too much fluid in the joint space, and decreased range of motion. There may or may not be pain when the cat’s affected joint is moved by you or your veterinarian.

Diagnostic Imaging
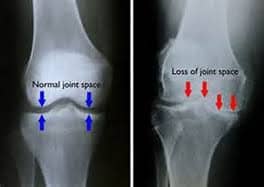
Radiographs and CT scans may show the excess fluid in the joints; the bony spurs; signs of an underlying disorder, such as elbow dysplasia, osteochondritis dissecans, hip dysplasia, or cruciate ligament rupture; and so forth.
Kinetic Tests
Force plate gait analysis in dogs can help find where the lameness is within the joint. It can also show the severity of lameness, both before and after therapy. A force plate is mounted to the floor, and the dog walks over it. Measurements are taken to see which areas use the least force (more affected) and vice versa. The gait analysis hasn’t been used as often in cats.
Therapeutic Trial
In some cases, a therapeutic trial of nonsteroidal anti-inflammatory drugs (NSAIDs) or a newer class of NSAIDS such as the brand name Galliprant may help confirm the diagnosis if the lameness is less noticeable after taking them.
Treatment, Management, and Prevention
It is not possible to cure arthritis.
The goals are to alleviate your pet’s discomfort, to minimize further degenerative changes to the joint, and to restore the joint’s functionality. Multiple types of treatment are usually necessary to relieve pain, stiffness, and discomfort.
Managing your pet’s weight is important. Excess weight increases stress on the joints and muscles. If your pet is obese, your veterinarian will want your pet to lose weight. Daily, low-impact activities, such as walking and swimming, will not only help your pet with losing some pounds but can also improve joint mobility, muscle mass, and exercise tolerance.
Joint supplements known as chondroprotective agents will help support the cartilage and will have some anti-inflammatory effects. These agents will slow the breakdown of cartilage and/or provide the building blocks that can help build it. Some agents also increase joint fluid secretion and thus decrease inflammation.
The main components of chondroprotective agents are polysulfated glycosaminoglycan (PSGAG), glucosamine, and chondroitin sulfate. Oftentimes there is no improvement using chondroprotective therapies. The failure may be due to too little cartilage left in the affected joint as there’s bone on bone; unresponsive joint inflammation; variable bioavailability of the drug between different products; and the lack of analgesia.
Although the injectable PSGAGs are more expensive, they provide a faster and longer-lasting response than the oral forms. If there is no response after 4-6 weeks, your veterinarian may discontinue use of PSGAGs.
Diets containing omega-3 fatty acids may help reduce inflammation. Some studies have found that dietary supplementation with fish oil omega-3 fatty acids can improve the clinical signs of arthritis in dogs, and may allow the NSAID dose to be reduced.
NSAIDS are an important component of arthritis therapy in dogs. Side effects that you should be aware of include stomach upset, elevated liver enzymes, and potential worsening of chronic kidney disease. Few NSAIDs are licensed for use in cats; your veterinarian will advise you about what NSAID options are available for your cat.
Analgesics such as tramadol, gabapentin, and amantadine may provide pain relief in dogs.
Alternative therapies such as acupuncture, stem cell therapy, platelet-rich or conditioned plasma, physical therapy, rehabilitation therapy (e.g. radial shock wave therapy, pulsed signal therapy), green-lipped mussel supplements, vitamin E, and zoledronic acid may be beneficial in some canine patients. Studies to support their use are still being done.
Surgery
Your veterinarian may consider surgical options if your pet’s response to medical treatment is low. In addition, your veterinarian may suggest surgery for certain underlying causes of arthritis, such as cranial cruciate ligament rupture, elbow dysplasia, osteochondritis dissecans, joint incongruity, intra-articular fractures, and joint instability.
Reconstructive procedures can eliminate joint instability and correct the anatomic defects. If your pet has severe hip dysplasia, your veterinarian may suggest a total hip replacement and femoral head/neck ostectomy. If the arthritis is in the wrist or ankle (then joint fusion may be considered; this surgery is usually well tolerated and can result in reasonable functionality.
Monitoring and Prognosis
Your veterinarian may need to do periodic physical examinations every 1-4 months to monitor your pet’s response to therapy and the progression of the disease. In addition, if your pet is on an NSAID, blood tests including complete blood counts and biochemistry profiles, should be done every few months to ensure there are no side effects impacting the liver or kidneys.
With therapy and careful monitoring, arthritis can be managed in many dogs and cats, resulting in a good quality of life that you and your pet will appreciate.
